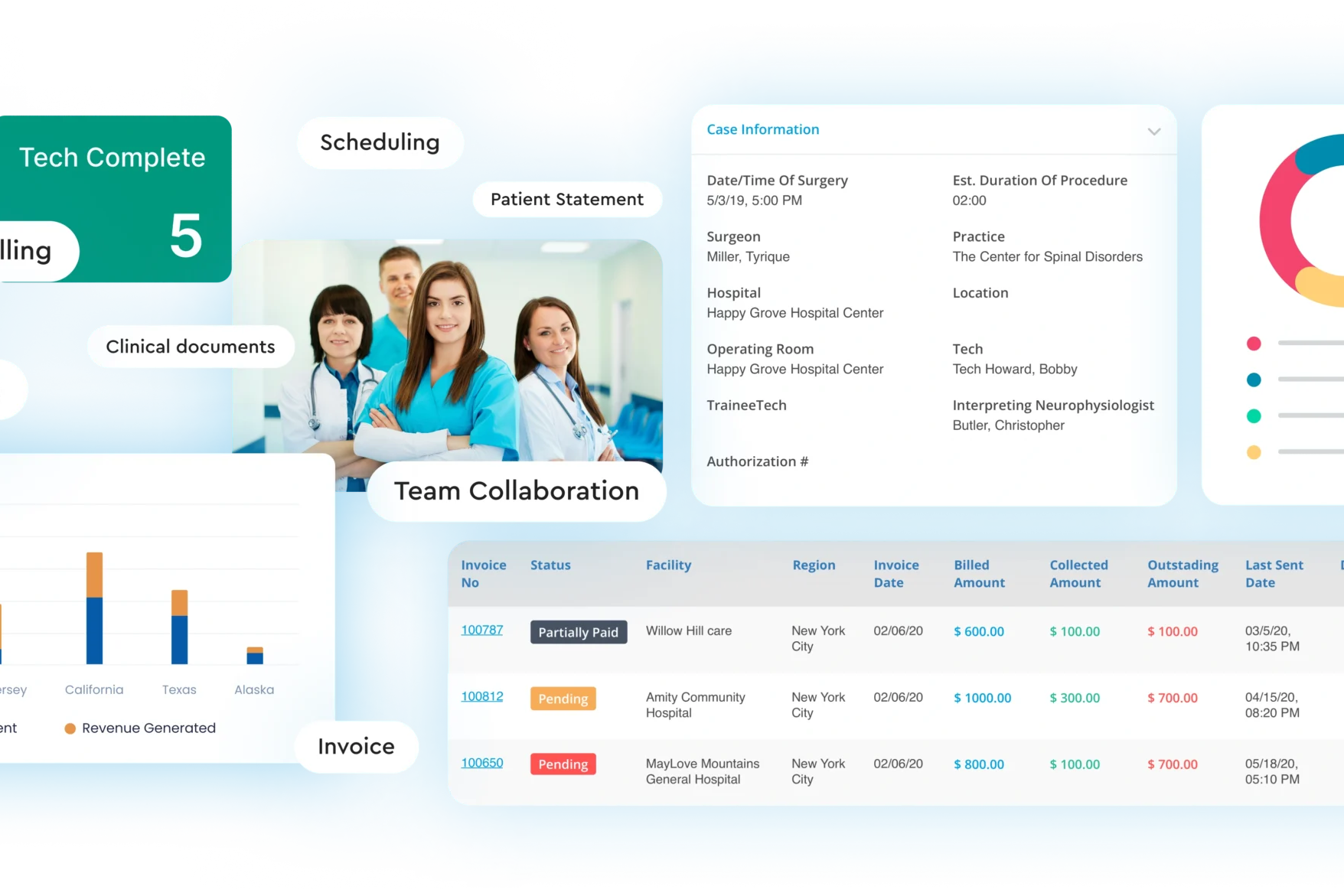
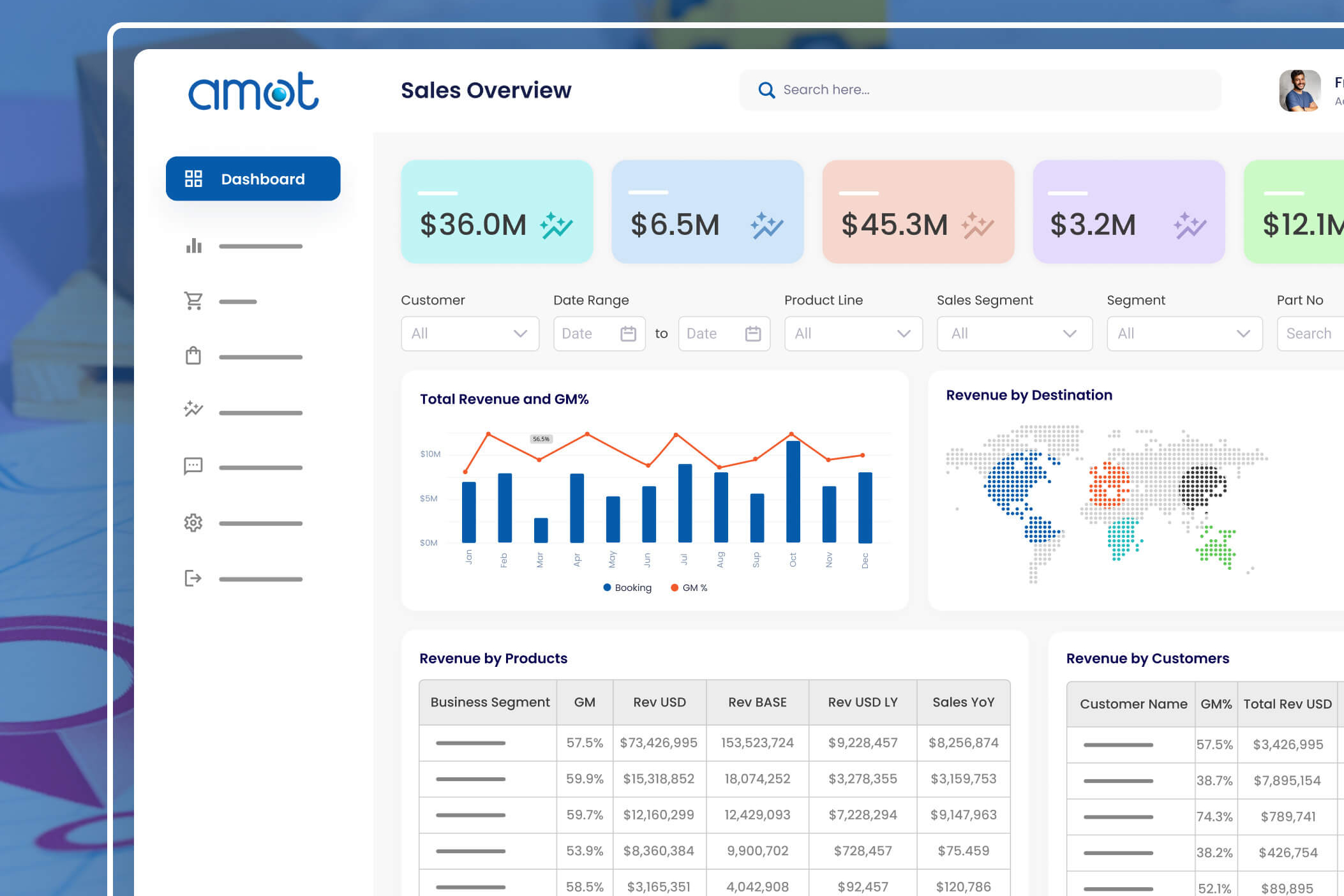
Remember those days? Stacks of paper threatening to topple over, the maddening hold music as you waited for a payer representative, and the sinking feeling of yet another denied claim landing on your desk? Those were the “good” old days of Revenue Cycle Management (RCM). Or, perhaps, not so good.
Today, AI in RCM is no longer a futuristic idea- it’s a practical, proven force that’s transforming how revenue flows through healthcare. From the patient’s first appointment to that elusive final payment, artificial intelligence is helping us move faster, make fewer mistakes, and create a better patient experience.
Why does this matter? The promise is real: faster payments, fewer errors, happier patients, and less burnout for our RCM teams. This isn’t about replacing human expertise; it’s about giving our teams AI-powered tools that make their work smarter, more strategic, and less stressful.
How We Got Here
Before AI came into the picture, RCM in medical billing was a labor-intensive marathon. We were managing a workflow that felt stuck in the last century, paper-based claims stacked on desks, endless spreadsheets, and entire teams dedicated to manual data entry. Every claim required multiple human touchpoints, and every delay had a ripple effect on cash flow. A single missing code or incorrect payer detail could mean weeks of back-and-forth with no guarantee of payment.
Today, nearly half of U.S. hospitals have adopted some form of AI in RCM. The result? Shorter revenue cycles, fewer denials, reduced operational costs, and a noticeable lift in patient satisfaction. The transformation is no longer theoretical, it’s happening in real time, and the organizations embracing it are setting a new benchmark for efficiency in healthcare finance.
How AI is Helping RCM Team Right Now

Turbocharging Eligibility & Benefits Verification
If there’s one bottleneck in the RCM in medical billing process that’s been universally frustrating, it’s eligibility and benefits verification. In the old model, staff spent hours, sometimes days- calling insurance companies, sitting on hold, and manually entering details into multiple systems. Every delay or oversight in this early stage had a compounding effect: incorrect coverage details could mean denied claims, delayed payments, and even tense conversations with patients who suddenly found themselves with unexpected bills.
This is where AI in RCM is changing the game. Modern AI-driven verification systems can:
- Run real-time eligibility checks directly with payers before services are provided.
- Identify coverage gaps or mismatches instantly, flagging them for review before a claim is even created.
- Cross-reference patient records with payer databases to confirm deductibles, co-pays, and out-of-pocket limits.
- Leverage healthcare AI agent chatbots to communicate with payer portals 24/7, pulling responses without tying up your staff.
The business impact:
- Denial rates drop because claims are cleaner from the start.
- The time your team spends on manual eligibility work shrinks dramatically.
- Staff can reallocate their energy toward higher-value tasks like patient engagement and revenue optimization.
Want to see it in action?
Our AI Call Agent can handle eligibility & benefits verification calls with payers in real time, no hold music, no manual note-taking, just instant results fed straight into your RCM workflow. Book Your AI Call Agent Demo Today
Smarter Medical Coding & Billing
If eligibility verification is the first line of defense in RCM in medical billing, accurate coding is the backbone. The coding process demands precision, a single wrong code can lead to claim rejections, delayed payments, compliance issues, or even audits. Traditionally, medical coders have relied on their deep knowledge and experience, manually translating physician notes and clinical documentation into standardized codes like ICD-10, CPT, and HCPCS. It’s a painstaking process, and even the best coders can be slowed down by the sheer volume and complexity of cases.
Some healthcare AI agent solutions can handle entire batches of charts without human intervention, processing thousands of encounters per hour. These systems also learn continuously, improving with each case and adapting to new documentation patterns or regulatory updates.
The business impact:
- Fewer errors: AI catches inconsistencies and missing documentation before a claim is submitted.
- Faster turnaround: Charts can be coded within minutes of service, accelerating the billing cycle.
- Improved compliance: Built-in checks help ensure every code meets payer and regulatory guidelines.
- More strategic focus: Coders can shift their time from repetitive code entry to reviewing complex cases, optimizing documentation, and advising on revenue opportunities.
Automated Denials Management
Denials are one of the most persistent headaches in RCM in medical billing. Every denied claim represents delayed revenue, additional administrative work, and frustration for both staff and patients. Traditionally, RCM teams would spend hours investigating why a claim was denied, digging through documentation, calling payers, and manually drafting appeal letters, all after the fact. By the time the claim was resubmitted, weeks or even months could have passed, impacting cash flow and operational efficiency.
With AI in RCM, the approach has shifted from reactive to proactive. Advanced algorithms can analyze historical claim data, payer behavior, and patient information to predict which claims are at risk of denial before they are submitted. This predictive capability allows your team to intervene early, correcting coding, verifying coverage, or obtaining missing documentation, before a claim ever reaches a payer’s desk.
The business impact:
- Reduced denial rates: Proactive intervention ensures more claims are approved on first submission.
- Faster cash flow: By minimizing delays and automating appeals, revenue cycles accelerate.
- Lower administrative burden: Staff spend less time on repetitive denial management and more on strategic revenue optimization.
- Increased patient satisfaction: Clean, accurate billing reduces confusion and improves trust.
Revenue Forecasting & Analytics
Historically, forecasting relied on spreadsheets, manual trend analysis, and educated guesses, a process prone to errors and limited in scope. Delays in understanding revenue trends could lead to staffing mismatches, resource misallocation, and missed financial opportunities.
With AI in RCM, forecasting has become far more precise and strategic. By analyzing historical payment data, claim patterns, seasonal trends, and payer behavior, AI models can predict future revenue with remarkable accuracy. These insights help leadership teams make informed decisions about staffing, budgeting, and capital allocation, reducing guesswork and increasing confidence in financial planning.
Modern healthcare AI agents can even simulate “what-if” scenarios. For example:
- What if a major payer changes reimbursement policies next quarter?
- How will delayed claims affect cash flow if patient volumes increase by 20%?
- Which departments might experience bottlenecks in billing cycles, and how should resources be reallocated?
The business impact:
- Data-driven decisions: Budgeting and resource allocation are informed by predictive analytics, not guesswork.
- Improved financial stability: Early insights help mitigate cash flow disruptions and reduce risk exposure.
- Strategic planning: Leaders can plan expansions, investments, or operational changes with confidence.
- Operational efficiency: Teams can anticipate workload spikes and prevent revenue bottlenecks.
Personalized & Painless Patient Payments
Billing and payments have long been a pain point for patients and providers alike. In traditional RCM in medical billing, patients often receive statements that are confusing, delayed, or inaccurate. This not only frustrates patients but also increases the likelihood of late payments, disputes, and bad debt, all of which strain the revenue cycle and your team’s time.
With AI in RCM, the patient payment experience is being transformed. AI can generate accurate cost estimates upfront, letting patients know what they owe before a procedure. It can automate reminders for upcoming payments or outstanding balances, reducing missed deadlines without requiring staff intervention.
The role of healthcare AI agents is particularly powerful here. They can:
- Answer billing questions instantly, 24/7, without putting patients on hold.
- Clarify insurance coverage, deductibles, and co-pays.
- Guide patients through online portals for secure payments.
- Escalate complex issues to human staff only when necessary, freeing your team for higher-value work.
The business impact:
- Higher patient satisfaction: Transparent, proactive communication builds trust and reduces frustration.
- Reduced bad debt: Accurate estimates and personalized plans increase the likelihood of timely payments.
- Operational efficiency: Staff spend less time on routine billing inquiries, allowing focus on exceptions and strategic initiatives.
- Revenue predictability: Fewer disputes and delayed payments improve cash flow consistency.
Fraud Detection & Compliance
A single fraudulent claim or compliance lapse can lead to financial loss, regulatory penalties, and a damaged reputation. Traditional monitoring relied on periodic audits, manual cross-checking of claims, and reactive investigations- a labor-intensive process that often caught issues too late.
With AI in RCM, the approach has become proactive and intelligent. Advanced algorithms continuously monitor billing patterns, cross-referencing patient records, payer data, and historical trends to detect anomalies that could indicate fraud or misuse.
Key capabilities of AI in fraud detection and compliance include:
- Real-time anomaly detection: Identify suspicious billing patterns as they occur, not months later.
- Automated risk scoring: Prioritize high-risk claims for human review.
- Continuous learning: AI models improve over time, adapting to new fraud schemes and changing regulations.
- Audit trail creation: Every action is logged, making regulatory reporting simpler and more transparent.
The business impact:
- Fewer compliance risks: Automated monitoring ensures adherence to regulations without relying solely on human oversight.
- Reduced penalties: Early detection prevents costly fines and audits.
- Stronger reputation: Demonstrating robust compliance and fraud prevention enhances trust with payers, regulators, and patients.
- Operational efficiency: Staff can focus on strategic initiatives rather than repetitive compliance checks.
Streamlining Post-Service & Admin
Once a claim is submitted, many organizations assume the heavy lifting is done. In reality, post-service administrative tasks, from payment posting to patient follow-up, can consume a significant portion of RCM resources.
AI in RCM is transforming this stage by automating these routine post-service processes. Using intelligent workflows and healthcare AI agents, organizations can:
- Automate payment posting directly from payer remittance advice, reducing errors and reconciliation delays.
- Flag and resolve discrepancies automatically, ensuring that underpayments or misapplied funds are quickly corrected.
- Send automated patient reminders and follow-ups, personalized to each patient’s billing situation.
- Provide instant responses to billing inquiries via AI-powered chatbots, freeing staff to focus on complex cases or high-priority accounts.
The business impact:
- Shorter A/R cycles: Faster payment posting and proactive follow-ups accelerate cash flow.
- Improved patient engagement: Automated, clear, and timely communication fosters trust and satisfaction.
- Reduced operational burden: Staff can spend their time on tasks that truly add value to the revenue cycle.
- Scalable operations: AI allows your RCM team to handle higher volumes of post-service activity without additional headcount.
Small and medium-sized businesses (SMBs) face unique challenges in supply chain management that can impact their operational efficiency, profitability, and consumer satisfaction. Power BI supply chain dashboards offer valuable solutions to address these challenges and empower SMB decision-makers to make informed decisions. Here are some common challenges faced by SMBs in supply chain management and how Power BI dashboards can help solve them:
- Limited Visibility and Transparency:
- Challenge: SMBs often lack visibility into their supply chain processes, making it difficult to track inventory levels, monitor supplier performance, and identify potential bottlenecks or issues.
- Solution with Power BI: Power BI dashboards provide real-time visibility into key supply chain metrics and performance indicators. Decision-makers can access interactive visualizations that offer insights into inventory levels, order statuses, and supplier performance, enabling them to make data-driven decisions and optimize supply chain operations.
- Inefficient Inventory Management:
- Challenge: SMBs may struggle with managing inventory levels effectively, leading to stockouts, overstocking, and excess carrying costs.
- Solution with Power BI: Power BI dashboards enable SMBs to monitor inventory levels, track demand patterns, and analyze inventory turnover rates. Decision-makers can use visualizations to identify slow-moving inventory, forecast demand more accurately, and optimize inventory levels to minimize carrying costs while ensuring product availability.
- Poor Supplier Performance:
- Challenge: SMBs may face challenges related to supplier reliability, quality issues, and delivery delays, impacting production schedules and customer satisfaction.
- Solution with Power BI: Power BI dashboards allow SMBs to track supplier performance metrics such as on-time delivery rates, quality control metrics, and lead times. Decision-makers can use visualizations to identify underperforming suppliers, address quality issues, and establish strategic partnerships with reliable suppliers to ensure a seamless supply chain flow.
- Lack of Data-driven Decision-making:
- Challenge: SMB decision-makers may rely on intuition or outdated information when making supply chain decisions, leading to suboptimal outcomes.
- Solution with Power BI: Power BI dashboards provide SMB decision-makers with access to real-time, accurate data and actionable insights. By analyzing key supply chain metrics such as order fulfillment rates, transportation costs, and inventory turnover, decision-makers can make informed decisions to optimize supply chain cycles, reduce costs, and improve overall efficiency.
- Difficulty in Identifying Trends and Patterns:
- Challenge: SMBs may struggle to identify trends, patterns, and opportunities for improvement within their supply chain processes.
- Solution with Power BI: Power BI dashboards enable SMBs to visualize supply chain data and identify trends, patterns, and anomalies. Decision-makers can use interactive visualizations to conduct root cause analysis, detect emerging trends, and implement proactive measures to address issues and capitalize on opportunities for improvement.
- Limited Resources for IT Infrastructure and Analytics:
- Challenge: SMBs may have limited resources and expertise to invest in sophisticated IT infrastructure and analytics solutions.
- Solution with Power BI: Power BI offers a user-friendly and cost-effective solution for SMBs to implement supply chain analytics. With its intuitive interface and cloud-based deployment options, SMBs can quickly deploy Power BI dashboards without the need for extensive IT infrastructure or specialized expertise, enabling them to harness the power of data analytics to drive supply chain improvements.
Not Sure Where to start with AI in Your RCM?
Book our Healthcare AI Agent Discovery Workshop to identify the best workflows to automate- boosting efficiency, reducing denials, and accelerating cash flow.
Opportunities & Challenges

What's Next for AI in RCM?
If today’s AI in RCM feels impressive, the next wave will feel like a complete reinvention of the revenue cycle. The evolution won’t just make processes faster, it will make them smarter, more adaptive, and more human-friendly.
Hyper-automation of nearly every RCM process
We’re moving toward an era where denial management, claims submission, payment posting, prior authorizations, and even follow-ups will be handled end-to-end by AI. These systems will operate around the clock, dramatically shrinking turnaround times and improving first-pass resolution rates.
Autonomous coding becoming the norm
While computer-assisted coding is already here, the future is fully autonomous coding that can interpret clinical notes, assign accurate codes, and flag anomalies without human intervention, all while maintaining compliance with changing regulations.
Specialized AI agents targeting each RCM task
Instead of one generic AI tool, we’ll see “micro-specialists”, AI agents fine-tuned for specific workflows like denial appeals, eligibility checks, or audit preparation. Each will continuously learn from case histories, becoming more effective over time.
Seamless integration with EHRs and voice-enabled AI assistants
AI will no longer sit as a bolt-on tool. It will live inside EHR systems, enabling real-time insights and actions. Voice-enabled AI assistants will let staff request data, check claim statuses, or schedule follow-ups simply by asking, speeding up work without touching a keyboard.
More personalized patient billing experiences
AI will help create tailored payment plans, send reminders in a patient’s preferred channel, and even provide predictive insights about who might need financial counseling before bills become delinquent, improving collections and patient satisfaction in one move.
AI delivered “as-a-service” for smaller providers
Historically, AI in RCM was a big-hospital luxury. The future will see cloud-based, subscription AI services making advanced automation accessible to clinics and mid-sized providers without heavy upfront investment, leveling the playing field across healthcare.
The big takeaway? RCM will shift from a reactive, manual-heavy process to a proactive, AI-orchestrated system where delays, errors, and inefficiencies are the exception, not the rule. The winners will be providers who adopt early, experiment often, and keep humans at the center of the AI loop.
Conclusion
This shift to AI-powered Revenue Cycle Management (RCM) isn’t a passing trend, it’s the new baseline for operational excellence in healthcare finance. The organizations that thrive in the coming years will be those that utilize AI not just for automation, but for insight, foresight, and patient experience transformation.
Our responsibility as leaders is clear:
- Equip our teams with intelligent tools that support, not replace, their expertise.
- Ensure AI adoption is ethical, transparent, and secure.
- View AI as a strategic partner, not just a cost-saving measure.
Ready to transform your RCM operations with AI?
Our healthcare AI experts at Sunflower Lab are here to help you assess, design, and implement intelligent solutions tailored to your needs. Contact our Healthcare AI Experts today and start leading in the era of intelligent RCM.
You might also like
Stay ahead in tech with Sunflower Lab’s curated blogs, sorted by technology type. From AI to Digital Products, explore cutting-edge developments in our insightful, categorized collection. Dive in and stay informed about the ever-evolving digital landscape with Sunflower Lab.