RCM Automation with Power Automate Saves over 200 Hours Daily across Departments

Say Hello!
A leading provider of Intraoperative Neuromonitoring (IONM) services, combining clinical expertise with real-time technology to enhance surgical outcomes. Backed by a team of certified technologists and neurologists, they specialize in monitoring the spinal cord, brain, and peripheral nerves during surgery, delivering critical information to surgeons when it matters most
Services
– Revenue Cycle Management Automation
– Cadwell Process Automation
Technologies & Integration
– Power Automate Cloud
– Power Automate Desktop
 ♦
♦  ♦
♦  ♦
♦  ♦
♦  ♦
♦
 ♦
♦  ♦
♦  ♦
♦  ♦
♦  ♦
♦
 ♦
♦  ♦
♦  ♦
♦  ♦
♦  ♦
♦
The Pain Points
 Manual patient case data processing which took over 45 minutes per case
Manual patient case data processing which took over 45 minutes per case Overwhelming back log of patient case data after holidays/weekends
Overwhelming back log of patient case data after holidays/weekends Risk of delays & errors in Cadwell process due to integration with multiple third-party systems.
Risk of delays & errors in Cadwell process due to integration with multiple third-party systems.
We Implemented the Following Solutions to Solve Thier Challenge
Used Power Automate & multiple bots to automate Revenue Cycle Management end-to-end.
Automated physician and hospital data entry from HubSpot into ZinniaX to reduce manual duplication.
Delivered real-time visibility into bot activity, execution status, and case metrics using Power BI dashboards.
Seamless automation across platforms like ZinniaX, Revedy, UHC, Waystar, HubSpot, and Tennr

We Implemented the Following Solutions to Solve ORBA’s Challenges:
A data lake to pull tax and assurance data from various data sources like Thomson Reuters, IRIS, Windows and store it in a centralized location for historical reporting.
A data lake would facilitate the integration of this data, making it more accessible for Power BI reports & analysis.
Automation Ecosystem

⸻ PROBLEM #1
Manual Cadwell Process Was Time-Consuming and Error-Prone
 IONM technicians spend around 45-60 minutes per case manually extracting data, coding, generating output files, and uploading in the system.
IONM technicians spend around 45-60 minutes per case manually extracting data, coding, generating output files, and uploading in the system. With over 250 daily, this led to staff overload, delays, and increased error rates.
With over 250 daily, this led to staff overload, delays, and increased error rates.

 IONM technicians spend around 45-60 minutes per case manually extracting data, coding, generating output files, and uploading in the system.
IONM technicians spend around 45-60 minutes per case manually extracting data, coding, generating output files, and uploading in the system. With over 250 daily, this led to staff overload, delays, and increased error rates.
With over 250 daily, this led to staff overload, delays, and increased error rates.

⸻ PROBLEM #1
Manual Cadwell Process Was Time-Consuming and Error-Prone
Our Solution
Automated Patient Data Extraction & Coding Workflow
A polished, three‑step pipeline that pulls records from ZinniaX, processes studies via Cadwell & Revedy, and automatically updates coding artifacts (including CMS‑1500) back in ZinniaX.
Automated Patient Data Extraction from ZinniaX
Bots were configured to extract required files—system files, case data, and technician‑completed records—from the ZinniaX platform.
Processing via Cadwell & Revedy Integration
The extracted files were fed into Cadwell software (hosted on a virtual machine). JSON outputs and PDF reports generated by Revedy were automatically retrieved and processed.
Coding Automation & CMS Updates
Coding bots parsed Revedy outputs and updated CMS‑1500 forms, modality details, and labeled the cases appropriately within ZinniaX.
Automated Workflow with Power Automate that:
Triggers upon receiving a purchase receipt in Dynamics 365.
Fetches relevant information from Dynamics 365.
Automatically generates an inspection ticket in a SharePoint list.
Databricks Services:
It is a quick platform, and it has been used very thoroughly for reading and for writing and for accessing and for doing the scoring of the data.
Directly connects with Orba’s existing systems (IRIS, Thomson Reuters, Power BI) via APIs for unified data access.
⸻ PROBLEM #2
Complexity in Managing Physician Pay and Insurance Validation

As a healthcare service provider handling high volumes of neurosurgical procedures across multiple hospitals, they faced increasing complexity in Physician Compensation Management & Verification of Benefits (VOB) as:
 Manually calculating varied physician pay (based on payer type), especially across hundreds of cases per week, was time-consuming, error-prone, and lacked standardization
Manually calculating varied physician pay (based on payer type), especially across hundreds of cases per week, was time-consuming, error-prone, and lacked standardization Manual insurance eligibility and benefit checks across UHC (Universal Health Coverage) & Waystar created bottlenecks in pre-authorization workflows, delaying case approvals and billing.
Manual insurance eligibility and benefit checks across UHC (Universal Health Coverage) & Waystar created bottlenecks in pre-authorization workflows, delaying case approvals and billing.
⸻ PROBLEM #2
Complexity in Managing Physician Pay and Insurance Validation
As a healthcare service provider handling high volumes of neurosurgical procedures across multiple hospitals, they faced increasing complexity in Physician Compensation Management & Verification of Benefits (VOB) as:
 Manually calculating varied physician pay (based on payer type), especially across hundreds of cases per week, was time-consuming, error-prone, and lacked standardization
Manually calculating varied physician pay (based on payer type), especially across hundreds of cases per week, was time-consuming, error-prone, and lacked standardization Manual insurance eligibility and benefit checks across UHC (Universal Health Coverage) & Waystar created bottlenecks in pre-authorization workflows, delaying case approvals and billing.
Manual insurance eligibility and benefit checks across UHC (Universal Health Coverage) & Waystar created bottlenecks in pre-authorization workflows, delaying case approvals and billing.

Our Solution

Reader Pay Bot
 This bot was built to automate physician pay calculations using predefined business rules based on each payer type
This bot was built to automate physician pay calculations using predefined business rules based on each payer type It retrieved necessary case and payer data, applied appropriate compensation logic, and updated pay records, removing the need for manual tracking or spreadsheets.
It retrieved necessary case and payer data, applied appropriate compensation logic, and updated pay records, removing the need for manual tracking or spreadsheets.
VOB Automation Bots
Two specialized bots were developed:
 VOB – UHC Bot: Performed Verification of Benefits for all UHC cases.
VOB – UHC Bot: Performed Verification of Benefits for all UHC cases. VOB – Waystar Bot: Handled VOB for all other payer types, ensuring comprehensive coverage
VOB – Waystar Bot: Handled VOB for all other payer types, ensuring comprehensive coverage


Improved Performance
Reduced tax returns data retrieval time from minutes to 2-5 seconds, regardless of data volume (even for 136K+ records).
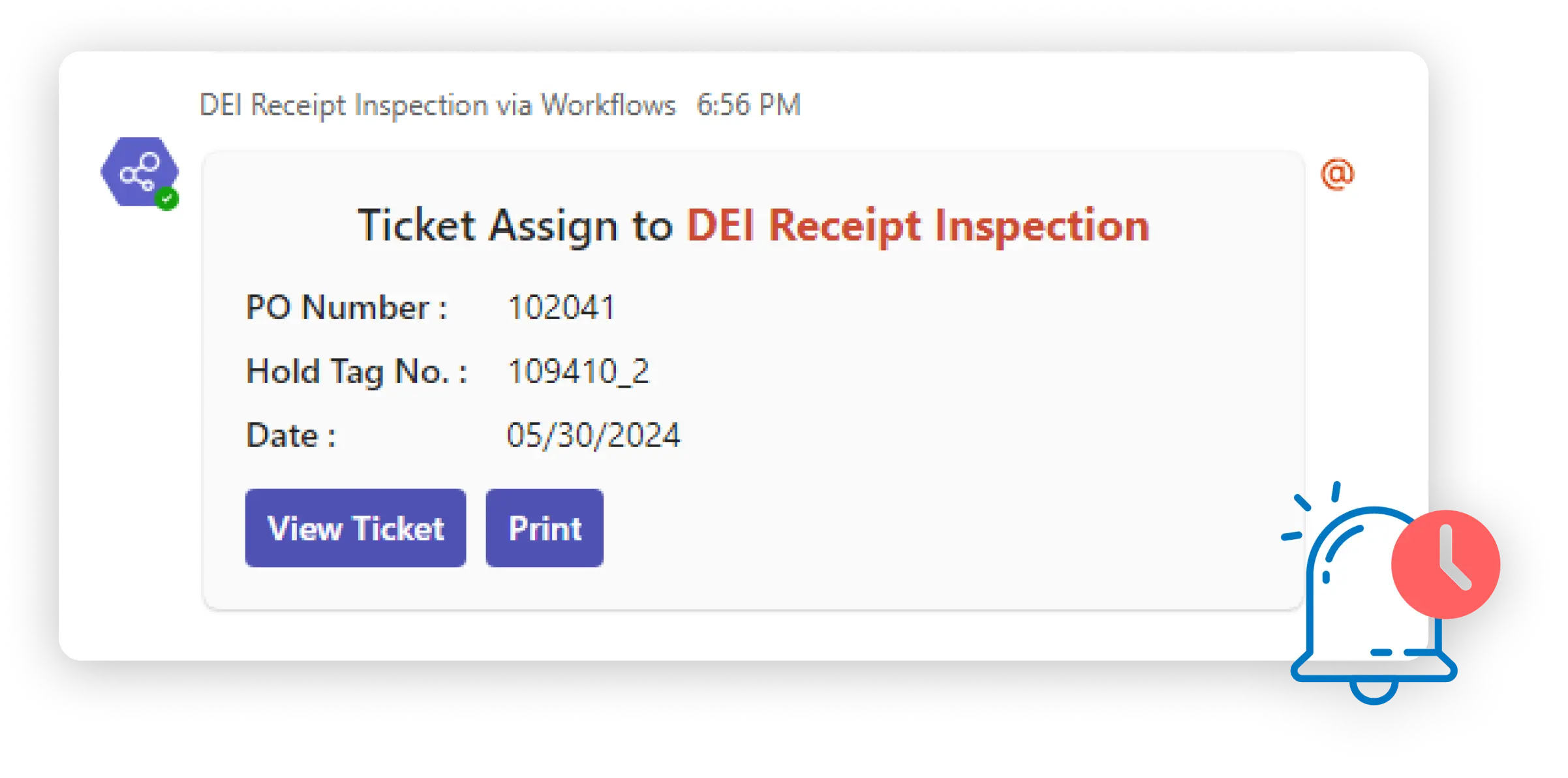
Automatic Notifications in teams
Improved Visibility: Inspectors receive instant notifications about new tickets, including priority ones, ensuring they’re aware of upcoming tasks and can plan their schedule accordingly.
Reduced Response Time: Real-time notifications eliminate delays in receiving information about new tickets. Inspectors can react quickly and prioritize urgent inspections.
Minimized Missed Inspections:The immediacy of Teams notifications significantly reduces the risk of missing or overlooking critical tickets, especially high-priority ones.
Reminders
Ensures Prompt Task Assignment: By reminding the assignor within 24 hours if a ticket remains unassigned, the system helps prevent tasks from getting stuck in limbo. This ensures inspections get assigned quickly and avoid delays.
Maintains Timely Status Updates: Reminding inspectors to update the status within 48 hours keeps everyone informed about the progress of inspections. This promotes transparency and helps identify any potential bottlenecks in the process.
⸻ PROBLEM #3
Delays During Holidays and Weekends Created Backlogs
When staff were unavailable, especially during long weekends, patient cases piled up and caused backlog and revenue delays.
Our Solution
24/7 Scheduling
 All mission-critical bots, especially those tied to the Cadwell workflow, verification of benefits (VOB), and reporting, were set up with automated schedules that execute daily or even multiple times a day.
All mission-critical bots, especially those tied to the Cadwell workflow, verification of benefits (VOB), and reporting, were set up with automated schedules that execute daily or even multiple times a day. This ensured that even if no human staff were available, these bots would continue processing patient cases as usual.
This ensured that even if no human staff were available, these bots would continue processing patient cases as usual.
Elimination of Backlogs
Previously, technicians would return on Mondays to a large backlog of unprocessed cases. With the bots running over the weekend, cases are now processed continuously, significantly reducing Monday load and enabling the team to start fresh.

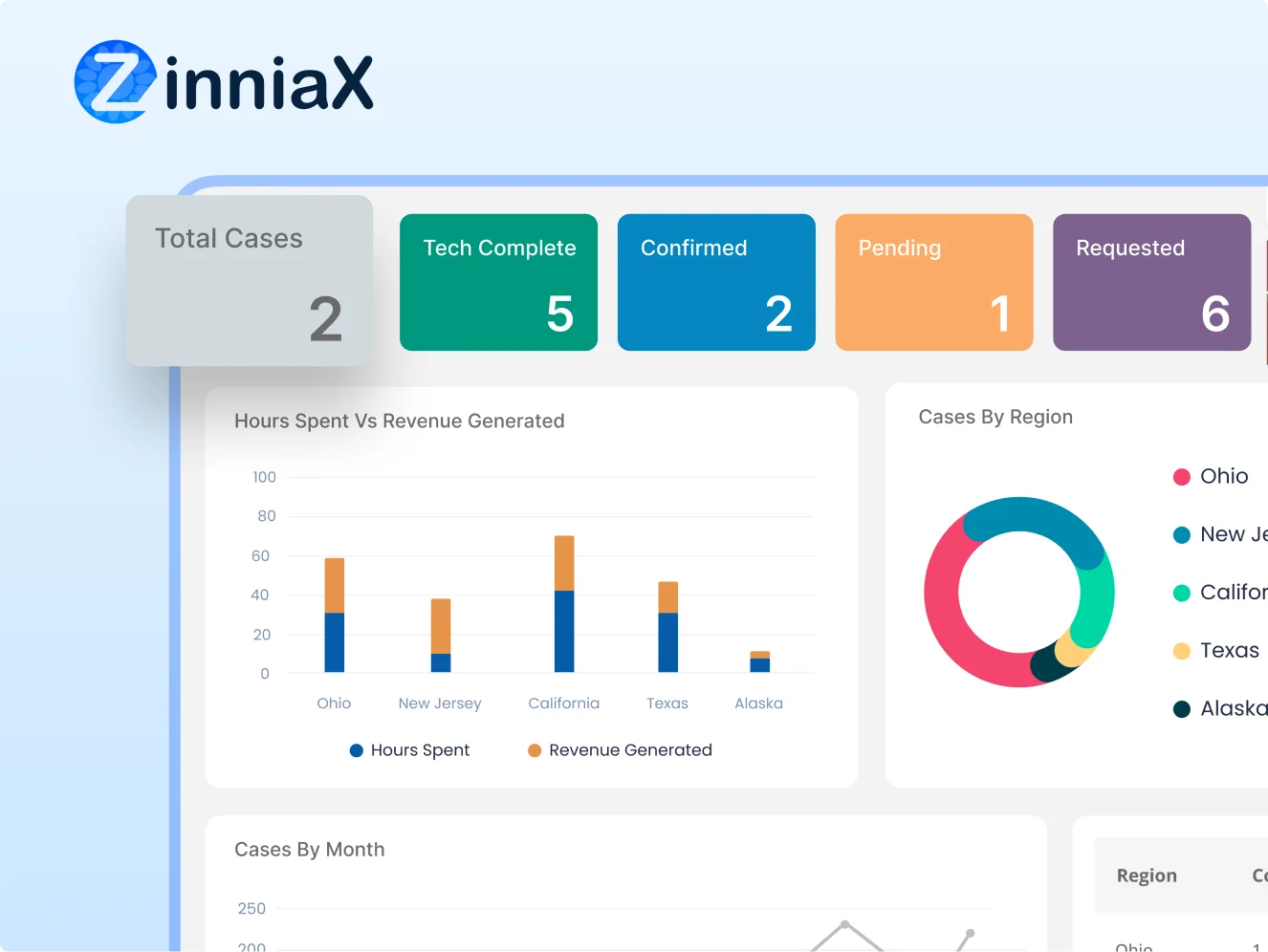
Bot Visibility & Case Progress Dashboard
Technical Personnel Dependency
As we automated critical workflows like Cadwell, Physician Pay, and Insurance Validation, we lacked visibility into bot operations:
- How many cases were processed
- When each bot last ran
- Whether the execution succeeded, failed, or was skipped
This information was hidden within Power Automate, accessible only by technical users—causing delays, bottlenecks, and disconnected teams.
Our Solution
We built a centralized dashboard accessible to both technical and non-technical staff, showing live bot activity and performance metrics.
| Bot Name | Last Run | Status | Cases Processed |
|---|
AI meets
Healthcare
AI-Powered Patient Engagement, Built for How Practices Work.
A HIPAA-compliant platform that automates patient communication, scheduling, insurance verification, and follow-ups — so clinical teams spend less time on admin and more time on care.
Where Sunflower Lab Stood Out?
Sunflower Lab proved to be the ideal partner for IONM provider’s automation and reporting challenges by combining technical expertise with a client-first approach. Here’s what set us apart

Process-First Mindset
We prioritized process understanding and reviewed detailed workflow diagrams with the thier team at every stage to ensure nothing was missed, and that both sides had a clear vision of how the automation would work.
The bots we built didn’t just automate tasks; they ensured business continuity by running 24/7, including weekends and holidays, allowing them to maintain operational flow even during staff downtime.

Rapid Responsiveness & Iteration
Whether it was bot maintenance, rule changes, or adding new workflows, Sunflower Lab was highly agile, quickly responding to evolving requirements and scaling automation alongside their growing needs.
Instead of leaving them in the dark, we built custom Power BI dashboards that gave full visibility into the automation performance, putting control back in hands of Operations & RCM teams.
Approximately 80% of healthcare organizations suffer revenue leakage due to RCM inefficiencies
Ready to Join the Elite 20% Healthcare Organizations?
You might also like
A SaaS Healthcare Product that Combines Data Analytics with Collaboration
Process Automation
HIPAA compliant archiving of healthcare data and report creation of patients
Power Apps, Power BI